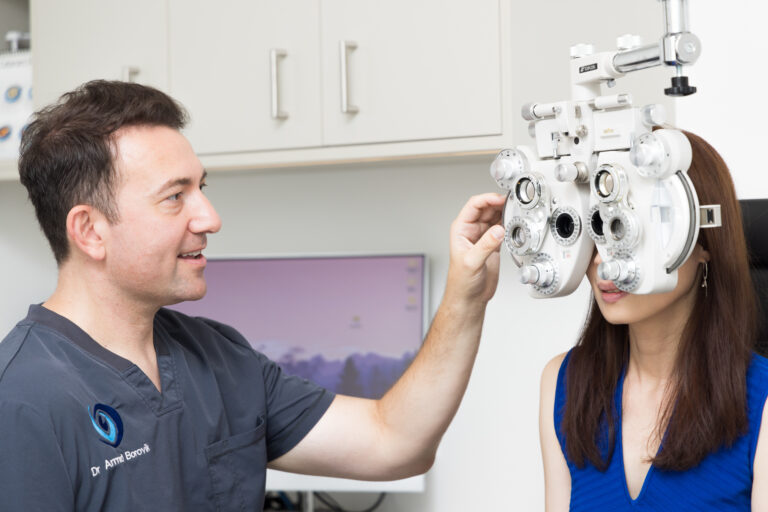
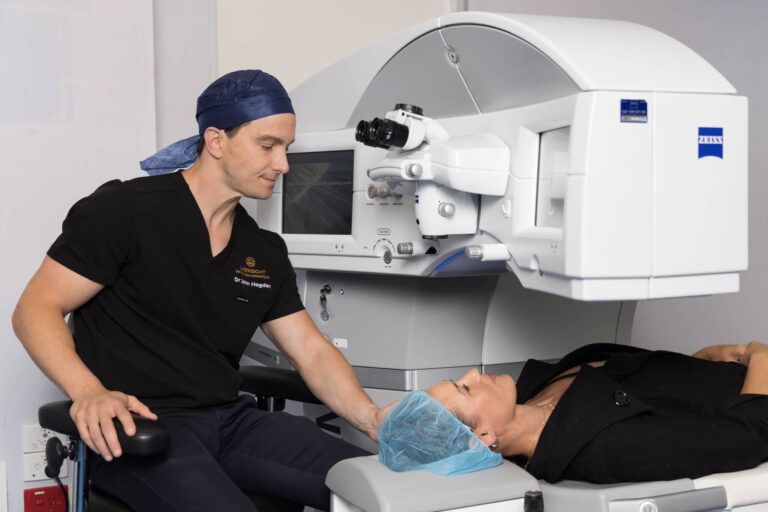
Keratoconus
We’ll strengthen your corneas to treat keratoconus.
Keratoconus is a progressive condition in which your cornea develops distortions such as bulges, or thins out. Our LASERLIGHT surgical teams use a combination of eyedrops and ultraviolet lights to stimulate growth and strengthening of the microscopic fibres in your cornea to overcome keratoconus.
Eyedrops and light
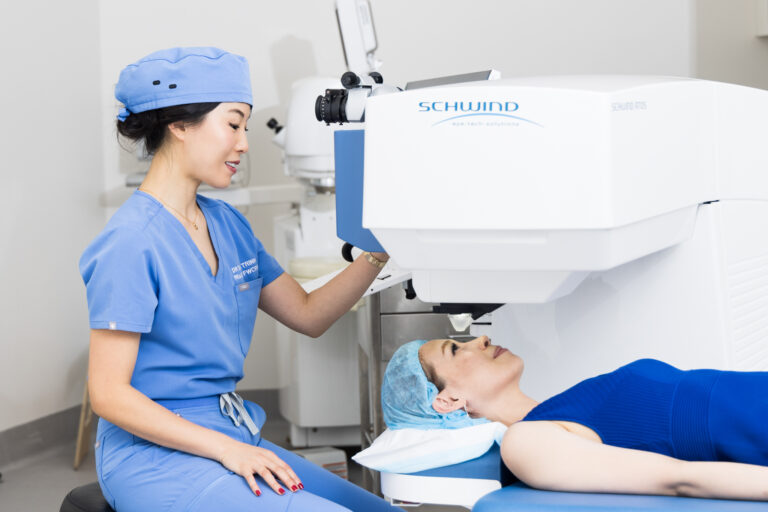
Your LASERSIGHT surgical team will conduct a thorough examination, and if cross linking is indicated, explain the procedure to you. We’ll carefully remove the outer layer of your cornea and use eyedrops containing collagen and riboflavin, activated by ultraviolet light, to strengthen your existing corneal fibres.
Experienced Surgeons and Advanced Technology
Our expertise in cross linking prescription and procedure completion is second to none, and we use the most sophisticated state of the art laser technology to ensure extreme accuracy.
Comprehensive Support and Follow-Up Care
From your initial consultation to long-term follow-up, we’re with you every step of the way, providing comprehensive care to make sure your eye care journey is smooth and successful.
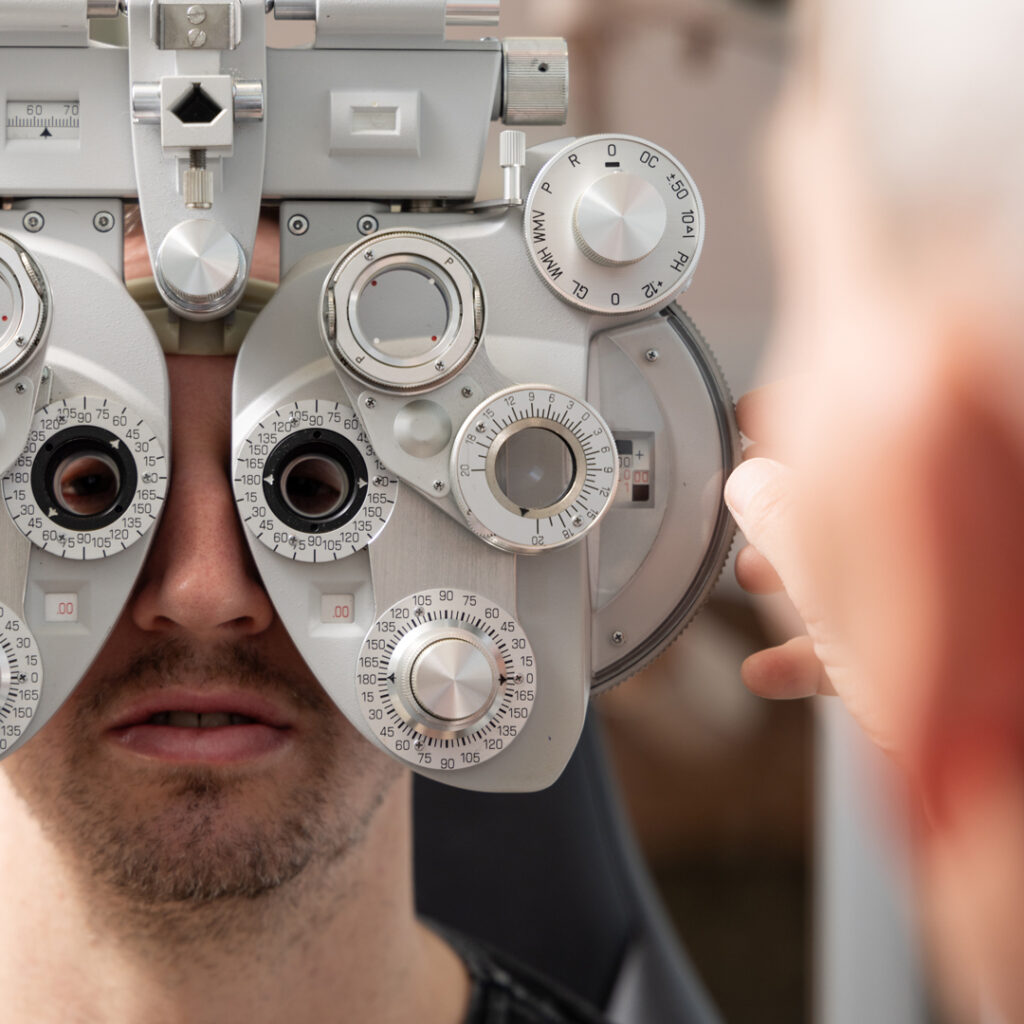
Will cross linking (CXL) work for you?
Personalised Care, Tailored Vision Solutions
Keratoconus tends to worsen over time, so the key is to get an early diagnosis and begin treatment. If your LASERSIGHT ophthalmology and surgical team recommend CXL, the chances of a full recovery are enhanced. However, cross linking may only slow development of the condition rather than stop it.
Procedure Time
Because of the nature of the procedure, you should be in the surgery for around one hour, allowing time for the strengthening process to take effect. From pre-op to post-procedure care, you’ll be ready to be picked up within two hours.
Typical Results
We will create a personalised treatment plan to ensure the best possible outcome. Whether the condition is slowed or stopped will depend on a range of factors, but our aim is to significantly improve your eyesight now and for the future.
Recovery Time
Following the procedure you will be fitted with temporary contact lenses that you’ll need to retain for several days. You may experience some dryness, a gritty feeling or some sensitivity to light, which can cause watery eyes, and the procedure itself may cause some discomfort. These symptoms usually subside within a few days as your eyes heal naturally, but you can take paracetamol to help.


LASERSIGHT by the Numbers
Proven Experience, Innovative Technology, and Personalised Care Delivering Exceptional Vision Correction Outcomes Across Australia.
Over three decades of leadership in laser vision correction.
Vision corrected for thousands of satisfied patients nationwide.
Cutting-edge treatments tailored to diverse vision needs.
Convenient locations across Australia offering expert care.
Our LASERSIGHT Locations
Trusted Across Australia
With clinics in key locations, we provide personalised laser eye surgery across New South Wales, Queensland, and Victoria.
Meet your Surgeon
Expert Surgeons, Personalised Vision Solutions
Discover the skilled surgeons dedicated to delivering exceptional care and vision correction tailored to your needs and goals.
Related Conditions
Discover the vision conditions treated with this service.
How much is laser eye surgery?
You’re currently paying with your time, money, and freedom to maintain your glasses and/or contacts. Is it really worth it?
Laser Eye Surgery Tips & Advice
Our team are committed to giving you the best advice
Popular resources
Our team are committed to giving you the trusted resources
Select your preferred Clinic
Let’s take the first step toward clearer vision.
Join over 90,000 Australians who trust us with their vision.